This Matrix From MIT Explains the COVID-19 Risk Level of Different Activities
Safely seeing people is much more nuanced than just staying six feet apart and donning your mask. Researchers created this COVID-19 risk level chart.

Safely seeing people is much more nuanced than just staying six feet apart and donning your mask. How crowded the space is, how loudly everyone is speaking, and what the ventilation is like can all impact your COVID-19 risk level. To make it less confusing, researchers at the Massachusetts Institute of Technology created a handy matrix chart.
Experts in This Article
chief medical officer of the Association of State and Territorial Health Officials
“It’s not just 6 feet and then everything else can be ignored or just mask and everything else can be ignored or just ventilation and everything else can be ignored,” Lydia Bourouiba, an associate professor of civil and environmental engineering at MIT and co-author of the report, told NBC. “[This chart] is a way to synthesize and, in some sense, translate complex notions into what we hope is an accessible color-coded chart.”
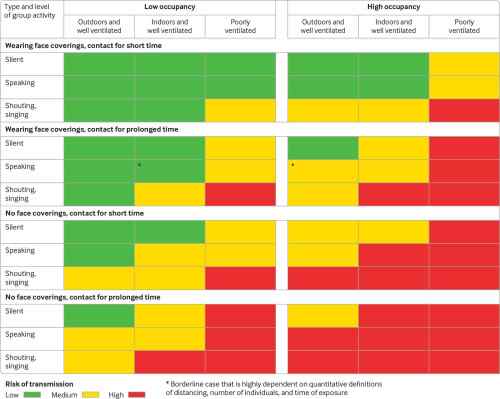
The report, published Tuesday in The BMJ, explains that physical distancing rules would be most effective if they reflected graded levels of risk. This chart Is based on the assumption that everyone is asymptomatic. For those with symptoms, they should be self-isolating meaning this information doesn’t apply.
“In the highest risk situations (indoor environments with poor ventilation, high levels of occupancy, prolonged contact time, and no face coverings, such as a crowded bar or night club) physical distancing beyond [six feet] and minimizing occupancy time should be considered,” the report reads. “Less stringent distancing is likely to be adequate in low-risk scenarios.”
Keep in mind that the levels in the above COVID-19 risk level chart are relative “especially in relation to thresholds of time and occupancy,” the report reads. “And they do not include additional factors such as individuals’ susceptibility to infection, shedding level from an infected person, indoor airflow patterns, and where someone is placed in relation to the infected person. Humidity may also be important, but this is yet to be rigorously established.”
Marcus Plescia, MD, MPH, chief medical officer of the Association of State and Territorial Health Officials, tells Well+Good that the safest place to see people is outside. The best bet is to use your own outdoor space if you have it.
“If it’s your backyard, you can control how things go in the backyard, you can control how the furniture is laid out if you have stuff for people, whereas in a park or other place you may have a little less control over that,” he says.
And Connie Steed, MSN, RN, president of the Association for Professionals in Infection Control and Epidemiology, says to keep gatherings small.
“There’s some guidance out there that suggests [gathering with] less than 10 people,” says Steed. “Ten is a little bit too much for my taste. As a group gets bigger, people forget about that six-foot rule and they get closer together. In my experience with my family and my colleagues, personally I think six or fewer people works.”
The report explains that further work is needed to extend the understanding of the cut-off duration of exposures, the detailed study of airflow patterns, and the patterns and properties of respiratory emissions and droplet infectivity within them during various physical activities.
Sign Up for Our Daily Newsletter
Get all the latest in wellness, trends, food, fitness, beauty, and more delivered right to your inbox.
Got it, you've been added to our email list.










