Our editors independently select these products. Making a purchase through our links may earn Well+Good a commission
6 Myths About Monkeypox Doctors Need You To Stop Believing
After two years of a pandemic, you're not wrong to worry about another infectious disease. Let's debunk some of myths about monkeypox.
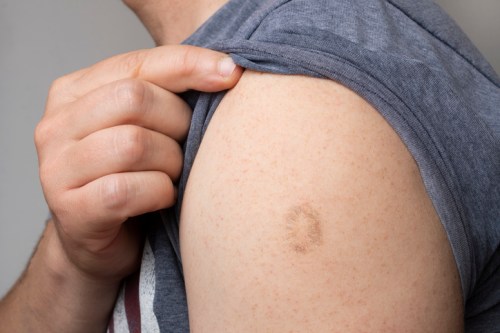
You’re not alone if you’re alarmed by headlines about monkeypox, a rare infectious disease in the smallpox virus family. The recently documented cases have left many of us with questions (and a considerable amount of misinformation to sort through).
First, let’s talk through the basics: Monkeypox spreads from animals to humans through direct contact with blood and bodily fluids from infected animals, according to the World Health Organization (WHO). However, it can spread among humans through skin-to-skin contact with an infected, inhalation of an infected person’s respiratory droplets (for long periods), and contact with materials that are contaminated by an infected person (like bedding and clothing).
Beyond tell-tale rashes and lesions (usually on the limbs and face), monkeypox symptoms include intense headaches, swollen lymph nodes, back pain, muscle aches, and fatigue, according to the Centers for Disease Control and Prevention (CDC). And though children are at greater risk for severe illness, most people who get monkeypox recover in two to four weeks, according to the WHO.
But what’s the latest cause for concern? Monkeypox is endemic, which means that it’s a disease which is consistently present but limited to specific geographic areas. Monkeypox outbreaks have recently occurred, however, in areas where it’s not commonly found. As of July 27, 2022, the CDC has documented 4,639 cases in the United States, with the highest number of cases in New York, California, Illinois, and Colorado.
While it’s reasonable to be concerned about monkeypox, especially against the backdrop of COVID-19, it’s equally important to be wary of myths and misinformation. To get some of the facts straight, let’s get the actual scoop from a virologist.
The Most Prevelant Monkeypox Myths
1. Monkeypox is a new virus (False)
“It is alarming to hear about new infectious diseases, especially after living through the COVID-19 pandemic or navigating HIV risk. However, monkeypox has been monitored, studied, and researched for years,” says molecular biologist Joseph Osmundson, PhD, a clinical assistant professor of biology at New York University and the author of Virology: Essays for the Living, the Dead, and the Small Things in Between.
Monkeypox was first documented in 1958 among research monkeys (hence, the name), and in 1970, cases among humans were discovered in the Democratic Republic of Congo and have been concentrated in Central and West African countries like Cameroon, Central African Republic, Gabon, Liberia, Nigeria, and Sierra Leone. There have also been occasional cases in Israel, Singapore, the United Kingdom, and the United States.
As a result, a significant body of information already exists, which some may find reassuring. For example, according to the WHO, the smallpox vaccine has efficacy against monkeypox, and there are existing developed vaccines. Additionally, there is also an existing antiviral medication. For more information about the monkeypox vaccine, visit the CDC’s website.
2. Monkeypox is a sexually transmitted infection (False)
“Even though it most commonly spreads through close contact with an infected individual, monkeypox is not an STI. Sex is just one example of close skin-to-skin contact,” says Dr. Osmundson. Holding hands, touching, hugs, or kissing are other ways monkeypox can spread. It’s also possible to spread the condition through body fluids or contaminated bed sheets and clothing, the WHO says.
Another reason monkeypox has been associated with STIs is because monkeypox symptoms can appear on the genitals. As a result, the CDC is asking STI clinics across the country to pay attention to their patient’s symptoms and watch out for cases. However, the virus is not considered an STI.
3. Monkeypox only affects gay and bisexual men (False)
The documented cases that we have seen have spread via international travel, two documented raves, and other situations that involve close, skin-to-skin contact (like sex). But remember, monkeypox is not an STI, and Dr. Osmundson says anyone could potentially contract it.
It just so happens that the recorded cases so far have disproportionately affected specific communities like men who have sex with men. However, this is correlative and doesn’t mean that it is a community-specific infection, says David C. Harvey, executive director of the National Coalition of STD Directors.
4. Monkeypox is the next COVID-19 (False)
Yes, monkeypox is concerning, but it is very different from COVID-19 in many ways. First, it is not a respiratory illness: It spreads through close contact with infected persons or particles, according to the WHO. While it can be spread by inhaling respiratory droplets from an infected person, it is not a disease that attacks the respiratory system like COVID-19.
Since the virus is part of the smallpox family, the vaccine for smallpox (that most adults in the U.S. born before 1970 received) is effective against monkeypox to some extent. If you’re curious if you’ve been vaccinated for smallpox, you can inquire about your vaccination status with a provider.
5. Monkeypox only affects people in African countries (False)
Many people on Twitter have pointed out that news outlets covering monkeypox are using photos of people of color—particularly Black people with cases of monkeypox. Although this has been a predominant visual trend, anyone of any race and skin color can contract the virus if they come into contact with an infected person.
It is true that the disease is most common in Central and West African nations, but that does not mean that it only affects people from these countries.
6. It’s ridiculous to worry about monkeypox (False)
The monkeypox virus does not resemble the features of COVID-19; however, some people have noticed dismissive reactions that mirror the way that some folks once talked about COVID-19. The truth is that it is okay to be worried about these cases.
Staying informed about the cases, the nature of the spread, and the communities that it is impacting is the best way to protect yourself—without feeling like there’s an insurmountable crisis brewing.
Sign Up for Our Daily Newsletter
Get all the latest in wellness, trends, food, fitness, beauty, and more delivered right to your inbox.
Got it, you've been added to our email list.










