Our editors independently select these products. Making a purchase through our links may earn Well+Good a commission
How hospitals and health care are getting a holistic makeover
Hospitals and medical systems are becoming increasingly open to a more holistic, integrative approach to care. Here's a look at a few leading the charge, including Donna Karan's Urban Zen Foundation.

It’s been fairly standard practice to head to your annual GP check-up with the goal of leaving as quickly as possible with a prescription in hand, no questions asked. But as holistic healing has become more mainstream, patients are increasingly seeking out other ways to treat their ailments first, whether it’s with herbs and food, acupuncture, energy healing, essential oils, or meditation. And so are doctors—and even some hospitals.
That’s because, the more studies are performed on alternative healing methods, the more evidence there is showing just how powerful they can be when worked into a treatment plan. But considering that many doctors aren’t trained—or even well-versed—in all the available options, the quest for holistic healing can be frustrating. According to one study, nearly half of patients are interested in complementary and alternative medicine, but less that 20 percent discuss it with their doctor. How do you know if reiki or acupuncture is best or which essential oil to use? And will your insurance cover your energy healing?
Slowly (and some would say, finally!) the traditional health-care system is changing to be more integrative, with healing not just referring to the injury or symptom, but the whole person as well.
Scroll down to see how health care is going holistic.
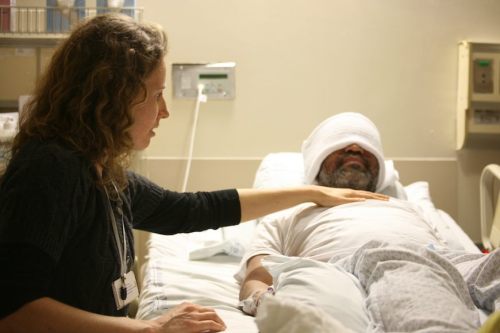
Where hospitals have traditionally fallen short—and how to fill the gap in your health care
As distinguished integrative health expert and How Healing Works author Wayne Jonas, MD, explains it, hospitals have historically been set up to handle things like health emergencies, surgeries, and manifestations of chronic illnesses, like if your arthritis flares up.
But according to a study by the Mayo Clinic, he writes, the top 10 reasons people see a doctor include ongoing, lifestyle-based issues like pain, fatigue, and hypertension. To truly heal these conditions, Dr. Jonas says, you need to think outside the pill bottle.
The top 10 reasons people see a doctor include ongoing, lifestyle-based issues like pain, fatigue, and hypertension. To truly heal these conditions, Dr. Jonas says, you need to think outside the pill bottle.
“Tell your doctor you want to integrate a more holistic approach and ask for what evidence-based [treatments] have shown to be successful,” says Dr. Jonas, who has also held the roles of director of the National Institute of Health Office of Alternative Healing and director of the World Health Organization for Traditional Medicine.
Our current health-care system may be “set up to make money while you’re sick,” says Dr. Jonas, but policies are changing, including those that affect the bottom line. “We need to make it more lucrative to stay well, and that includes payment structures and incentives that motivate people [to make healthy choices].”
One example he gives is health-care plans that offer a discount to people who wear a tracker and take more than 5,000 or 10,000 steps a day. He also says that’s why an increasing number of insurance companies are required to cover a “wellness visit,” which isn’t about treating disease, but staying healthy. This is something that companies like Parsley Health and digitally-born Maven Clinic have been championing outside the traditional health-care setting, because reforming the system itself has thought to be untenable.
That said, there are ways that holistic health is growing within American hospitals.

The rise of holistic care in hospitals
In the 1990s, a few pioneering hospitals opened their doors to alternative solutions. During this time, for example, Memorial Sloan Kettering Cancer Center began offering holistic treatments (including aromatherapy, acupuncture, and touch therapy—all priced à la carte) to patients and their families. And both Duke University Medical Center and the Mayo Clinic added acupuncture, massage, and other complementary and alternative medicine (CAM) services to their Rx pads. A decade later, in 2006, Yale joined the newly formed Academic Consortium for Integrative Medicine and Health. By 2008, U.S. News reported that all 18 institutions that made the Honor Roll on its list of “America’s Best Hospitals” provided CAM services.
In 2007, motivated by the death of her husband to cancer seven years earlier, fashion designer Donna Karan founded the Urban Zen Foundation with the mission to bring integrative treatments to hospitals across the country—since its inception, the program has significant partners in the medical community from Mount Sinai Beth Israel in New York to UCLA Medical Center.
Currently, over 800 certified specialists are part of the Urban Zen Integrative Therapy (UZIT) program, which “seeks to create the ultimate healing environment” by making five modalities—yoga therapy, reiki, essential oil therapy, contemplative care, and nutrition—available to both patients and health-care workers in hospitals.
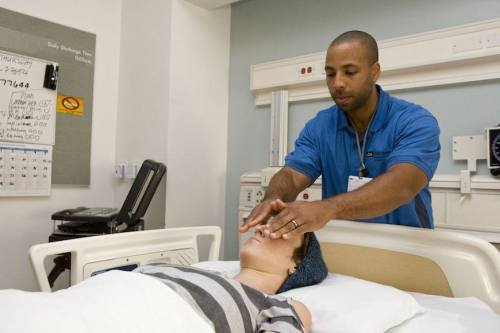
Designing hospitals for better health
Extending treatments to doctors, nurses, and hospital staff (such as those who work with cancer patients) has set UZIT apart from the programs that came before it. And it’s a major reason why CareRite Centers, a system of immersive rehabilitative centers with footholds in New York, New Jersey, Pennsylvania, Florida, and Tennessee, has partnered with Urban Zen in 10 locations.
Ashley Romano, CareRite’s national director of patient experience, says it was important for them to provide a way to care for their staff and prevent burnout among medical professionals. “They’re seeing everything from an amputee taking his first steps to a patient taking his last breath, so it’s very taxing,” she says. The industry data backs up her personal experience: According to a study by the Mayo Clinic, 54 percent of physicians reported at least one symptom of burnout in 2014, up from 45 percent in 2011. “So we introduced [UZIT] to our staff first, and then our patients,” Romano explains.
In many hospitals, Urban Zen is designing what they call “Zen dens,” calming rooms health-care workers can use to go over a perplexing case with a colleague, have difficult conversations with patients, or just take a breath alone. “It’s a place to find the calm in the chaos, as Donna [Karan] says,” executive program director Gillian Cilibrasi explains.
We have good scientific evidence that physical spaces influence healing for many chronic conditions.
There’s research to support that these well-designed rooms are more than just a space for healing—they are a means of healing in and of themselves. “Almost everyone knows the calming effect of a beautiful vista, a sunny day, or the sound of flowing water,” Dr. Jonas writes in his book. “We have good scientific evidence that physical spaces influence healing for many chronic conditions, and there is growing understanding of the mechanisms in our brain that do that.” He points to neuroscientist Esther Sternberg, MD, who spent 30 years investigating the links between stress and environment. She found that a physical environment directly impacts someone’s ability to heal, independently of what happens in the space.
Making changes to a healing environment isn’t confined to the hospital walls—it can be implemented at home. In fact, one of UZIT’s biggest benefits, both Romano and Cilibrasi stress, is that it helps heath-care providers and patients learn how to take their healing practices home with them. “We get patients emailing us about where they can buy a diffuser or get essential oils, or they come back and take a fitness class, which we offer to the community, and that’s really rewarding,” Romano says.

Why women have the power to change the medical system
Dr. Jonas says the medical landscape is at the tipping point of change. “It’s going to be the public that will start making demands,” he says. “We’ve already seen that happen in the food industry with the demand for healthier options.” And, he says, it’s really women who have the power to change the industry.
“The big secret is that it’s actually women who make the decisions in our health-care industry because they are frequently more active in their own lives and often in a position where they are taking care of children, the elderly, or their partners,” Dr. Jonas says. “If women start demanding more integrative health and have a collective voice around that, it will rapidly change.”
For UZIT’s Cilibrasi, seeing the impact firsthand is enough to keep her pushing forward. “It’s profound to be able to offer something else—not in place of traditional medicine but in tandem with it,” she says. “Instead of throwing medication at a patient, this is providing one-on-one care while helping them find a grounded moment.” First, energy work in the oncology unit; next, meditation in the OR? With the way things are trending, the idea—and many that haven’t even been hatched yet—seems completely within the realm of possibility.
While you explore the world of holistic health, here’s what you need to know about all the different wellness job titles and what they mean.
Sign Up for Our Daily Newsletter
Get all the latest in wellness, trends, food, fitness, beauty, and more delivered right to your inbox.
Got it, you've been added to our email list.










