‘I’m a Dermatologist, and These 7 Things Could Be Making Your Psoriasis Worse’
It's important to know what things can make psoriasis worse so you can try to avoid them the best you can. Learn about them here.
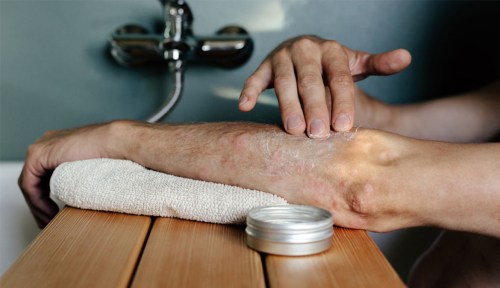
More than 125 million people worldwide deal with psoriasis and the itching and discomfort that comes along with it. The chronic inflammatory skin condition impacts the way skin cells mature, resulting in often red or pink flaky skin lesions where the skin barrier is broken. These dry patches can often seem to come out of nowhere, but according to Ivy Lee, MD, a board-certified dermatologist in Pasadena, California, there are certain things that can lead to flare-ups.
Experts in This Article
board-certified dermatologist
It’s important to note that psoriasis is a genetic condition, which means that if you have it, it’s not because you did something “wrong”—it’s simply because you’re predisposed. That said, there are a few factors that can make flare-ups worse, so you’ll want to be aware of what they are and do your best to avoid them. Keep scrolling for seven biggies that Dr. Lee wants you to look out for.
1. Friction
To avoid psoriasis flare-ups, Dr. Lee says it’s key to try to minimize points of friction. “I have players who wear knee pads and you realize their psoriasis is really bad underneath their knee pads, or I have women who wear bras with underwires and it’s really uncomfortable, really rubbing that area underneath the breast,” says Dr. Lee. “And you realize that their psoriasis is really concentrated, really angry, and flared underneath their breast. And that’s because there’s a little friction point that people are getting flares at.”
2. Cuts, scrapes, and exfoliation
“There’s a known phenomenon called the Koebner Phenomenon, where any type of trauma—so cuts, scrapes, even self-induced trauma, like a scratch or a rubbing—can flare your psoriasis,” says Dr. Lee. She explains that oftentimes patients with mild psoriasis will try to get rid of it by scrubbing the area with a loofah or pumice stone, and will then find that the scales got worse or spread to a larger area. “And that’s what we call the Koebner Phenomenon, where if you manipulate, scratch, or abrade your psoriasis, it can spread.”
3. Psychological stress
When you’re stressed out, your skin feels it. “It’s fascinating because we’re learning a lot more about the immunological basis of psoriasis and skin conditions like atopic dermatitis in eczema, and you realize that any type of inflammation and psychological stress can dampen or ramp up parts of our immune system,” says Dr. Lee. When this happens, conditions like psoriasis and eczema can flare as a response to that increased inflammation. “The mind and body are actually very connected,” she adds.
This Parisian Skincare Brand Is Launching in the United States for the First Time—Here’s What a Derm Wants You to Know

We’re Calling It: Cleansing Balms Are the Face Wash of the Future—Here Are 3 to Add to Your Cart

This Is the One Product That Scarlett Johansson Always Keeps in Her Purse and on Her Bedside Table

4. Physiological stress
In addition to mental stress, physical stress on your body can also have an effect on your skin. “For example, when I ask patients about their overall stress level, they think about their psychological stress and say, ‘I feel absolutely fine,’ but then they’re like ‘Oh wait, but I did have that surgery’ or ‘I was hospitalized for for a week for Covid,'” says Dr. Lee. “That physiological stress can also cause a flare of psoriasis”
5. New medications“Asking people about any new medications is really helpful because sometimes we realize it may not just be a flare of their regular psoriasis,” says Dr. Lee. “Maybe they started a new medication that maybe is flaring their current psoriasis or causing them to develop a rash that looks a lot like psoriasis.”
6. Cold weather
Although this isn’t true for everyone, cold weather has the potential to cause flare-ups. “There is a seasonality, usually around the winter months, where we do know chronic psoriasis patients may have a flare,” says Dr. Lee. “I have patients who say, ‘Every year from November to January is where my psoriasis flares.’ And it’s hard. I can’t predict who has this seasonality or why they have that seasonality. We think that maybe it’s because of the drier weather, the ambient humidity, and lack of moisture in the skin that’s causing the flares in psoriasis.”
7. Internal conditions
“We used to think that psoriasis was only on the skin and now we have a lot more information that it is associated with other conditions,” says Dr. Lee. “Psoriasis can affect arthritis. It can be associated with heart disease, heart attacks, and strokes. It can be associated with high blood pressure, diabetes, and high cholesterol—all these things that ideally we don’t want. And so we realize that it’s no longer just affecting the skin and that this is where skin maybe is one of the manifestations of all of this inflammation. We understand a lot more about how psoriasis affects the whole body, and we’re also a lot more proactive in finding any associated internal conditions that maybe we can prevent or treat at an earlier point.”
Want even more beauty intel from our editors? Follow our Fineprint Instagram account for must-know tips and tricks.
Sign Up for Our Daily Newsletter
Get all the latest in wellness, trends, food, fitness, beauty, and more delivered right to your inbox.
Got it, you've been added to our email list.







